Why Imprimis IVF Is the Best IVF Centre in Jammu and Kashmir for Complex Infertility Cases
Jammu & Kashmir, India – In a region where access to advanced fertility care has long been limited, Imprimis IVF is redefining reproductive healthcare with science-led treatments, ethical practices, and consistently strong outcomes, especially for complex infertility cases. With a growing footprint across India and a patient-first philosophy, Imprimis IVF has emerged as the most trusted IVF centre in J&K, offering hope to couples who were once told their chances were minimal.
This press release explores why Imprimis IVF stands apart, how it handles high-complexity fertility challenges, and what makes it the preferred destination for patients across Jammu & Kashmir and neighbouring regions.
Understanding the Rising Need for an Advanced IVF Centre in J&K

Infertility is no longer a rare concern. Medical data and on-ground realities indicate a steady rise in infertility cases due to late marriages, hormonal imbalances, PCOS, endometriosis, male factor infertility, stress, and lifestyle changes. In Jammu & Kashmir, couples often face an added challenge, limited access to tertiary-level fertility care, forcing many to travel outside the state.
Imprimis IVF bridges this gap by bringing metro-grade IVF technology and expertise to the region, ensuring patients receive world-class fertility treatment without the burden of long-distance travel.
Imprimis IVF Centre is Built for Complex Infertility Cases

What truly differentiates Imprimis IVF is its specialisation in complex and previously failed infertility cases. These include:
- Repeated IVF failures
- Low ovarian reserve (low AMH)
- Severe male infertility (azoospermia, oligospermia)
- Endometriosis and uterine abnormalities
- Advanced maternal age pregnancies
- Genetic or chromosomal concerns
- Unexplained infertility
Rather than offering a one-size-fits-all approach, Imprimis IVF follows deep diagnostic protocols, ensuring each treatment plan is customised to the patient’s biology and reproductive history.
Advanced IVF Technology That Matches Global Standards

At the core of Imprimis IVF’s success is its cutting-edge fertility infrastructure. The centre is equipped with:
- State-of-the-art embryology laboratories
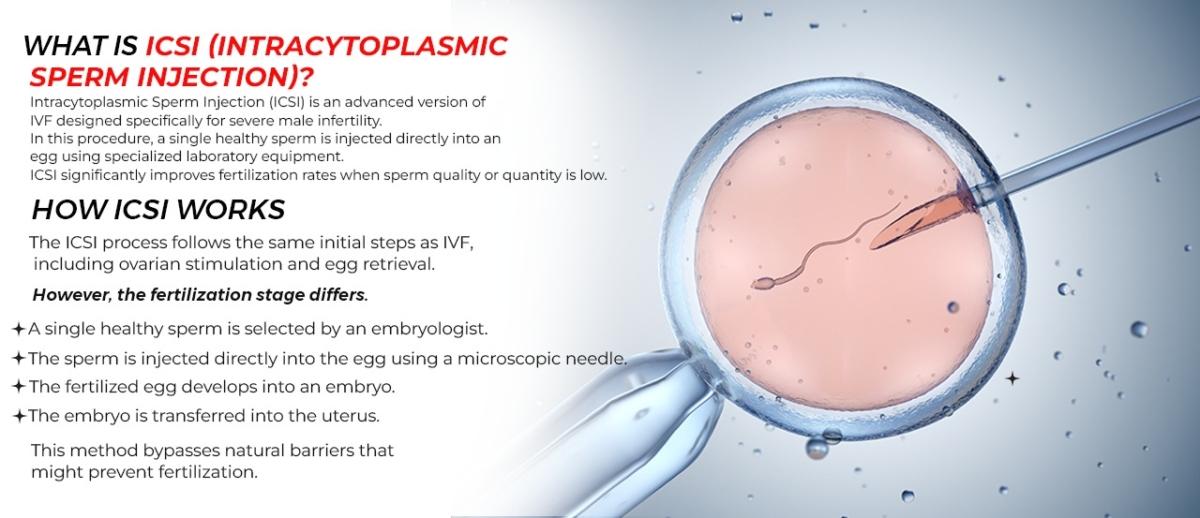
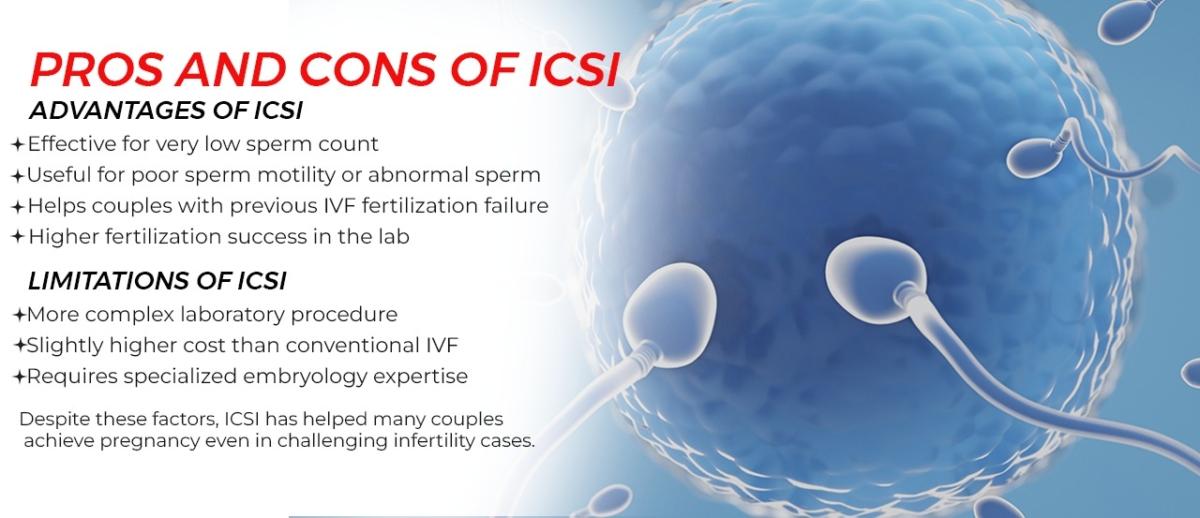
- Advanced ICSI and IMSI facilities
- Blastocyst culture and vitrification
- Time-lapse embryo monitoring
- High-end ultrasound and hormonal diagnostics
- Stringently controlled clean-room labs
These technologies significantly improve embryo selection, implantation rates, and overall IVF success, especially in medically challenging cases.
Highly Experienced Fertility Specialists and Embryologists – Imprimis IVF

Behind every successful IVF journey is an expert team, and Imprimis IVF prides itself on its highly qualified fertility doctors, embryologists, and clinical staff.
The centre’s specialists bring:
- Years of hands-on experience in handling high-risk infertility
- Training from leading national and international fertility institutions
- Strong expertise in reproductive endocrinology and embryology
This depth of clinical knowledge allows the team to anticipate complications early, adjust protocols in real time, and optimise outcomes, a critical factor in complex cases.
Evidence-Based, Ethical, and Transparent Treatment Protocols
In an industry where overpromising is common, Imprimis IVF takes a refreshingly ethical approach. The centre is known for:
- Clear communication of success probabilities
- Honest evaluation of each case
- Avoidance of unnecessary procedures
- Transparent pricing and counselling
Patients are guided with realistic expectations, empowering them to make informed decisions at every step of their fertility journey.
Personalised IVF: No Two Patients Are Treated Alike
One of the strongest pillars of Imprimis IVF’s success is its belief in personalised medicine. Each couple undergoes a comprehensive evaluation that includes:
- Hormonal profiling
- Genetic and metabolic screening (when required)
- Uterine and ovarian assessment
- Sperm DNA and functional tests
Based on these insights, the medical team designs tailored stimulation protocols, embryo transfer strategies, and supportive therapies, ensuring the highest chance of success for even the most complex cases.
High IVF Success Rates in Challenging Scenarios
While success rates vary depending on medical complexity, Imprimis IVF has consistently demonstrated encouraging outcomes in difficult cases, including patients with prior failed cycles elsewhere.
These results are driven by:
- Precision-driven protocols
- Advanced embryo selection techniques
- Continuous monitoring and protocol optimization
- High lab standards and quality control
For couples who have experienced repeated disappointment, this clinical excellence often becomes the turning point.
Emotional Support and Compassionate Care
Infertility treatment is not just a medical journey; it is an emotional one. Imprimis IVF recognises this deeply and integrates compassionate counselling and patient support into every stage of care.
Patients frequently highlight:
- Empathetic consultations
- Accessible doctors and care coordinators
- Respect for emotional and cultural sensitivities
- A non-judgmental, supportive environment
This holistic approach helps reduce stress, improve patient confidence, and foster a more positive treatment experience.
Accessibility for Jammu & Kashmir Patients
By establishing advanced IVF services within the region, Imprimis IVF has made high-quality fertility care accessible and affordable for couples in Jammu & Kashmir.
Key advantages include:
- Reduced travel and accommodation costs
- Continuity of care close to home
- Easier follow-ups and monitoring
- Family support during treatment
This accessibility has positioned Imprimis IVF as the first-choice fertility centre for local patients as well as those from nearby states.
Commitment to Continuous Innovation and Learning
Medicine evolves rapidly, and so does Imprimis IVF. The centre actively invests in:
- Latest fertility research and clinical updates
- Regular training and skill enhancement
- Upgrading laboratory and diagnostic technology
- Adopting globally accepted best practices
This commitment ensures that patients always receive current, evidence-backed treatments, not outdated protocols.
Trust Built on Results, Ethics, and Patient Stories
The reputation of Imprimis IVF is built not on marketing claims, but on real patient success stories, ethical practices, and consistent clinical outcomes. Word-of-mouth referrals, repeat patients, and long-term trust from the community speak volumes about the centre’s credibility.
For many families in Jammu & Kashmir, Imprimis IVF is not just a clinic; it is the place where hope was restored, and dreams of parenthood became reality.
Conclusion: Setting a New Benchmark for IVF Centre in Jammu & Kashmir
In a region that needed reliable, advanced fertility care, Imprimis IVF has raised the standard. With its expert medical team, world-class technology, personalised protocols, and ethical patient-first approach, it has rightfully earned recognition as the best IVF centre in Jammu & Kashmir for complex infertility cases.
For couples navigating the uncertainty of infertility, especially those facing medical challenges, Imprimis IVF stands as a beacon of trust, science, and compassion, offering not just treatment but a genuine chance at new beginnings.
Imprimis IVF Centre Branches: –
Best IVF Centre in Srinagar, Kashmir